Dr. Na Zhai Clinic Acupuncture & Chinese Medicine
Does Acupuncture really works?
I earned my bachelor’s and master’s degrees from Western medical institutions, and for a long time, I was a complete skeptic of Traditional Chinese Medicine (TCM), particularly acupuncture.
My disbelief was first challenged by a front-page article in a respected national newspaper. It reported on a remarkable clinical study from the Tianjin University of Traditional Chinese Medicine—China’s largest stroke treatment and research center. The article claimed that a unique acupuncture technique enabled 66% of 5,168 acute stroke patients to return to daily life, with some even resuming their jobs. I found this hard to believe; it seemed impossible.
Driven by sheer curiosity, I applied for a Ph.D. position at that very university. I was determined to uncover the truth: Did acupuncture induce a genuine physiological change in the brain, or was its effect merely psychological?
My research led to an innovative experimental design. To visualize cerebral circulation in rats, we injected a special red dye directly into the left ventricle of the heart while it was still beating. The heart’s own natural pumping force distributed the dye throughout the bloodstream, including to the brain. This method allowed us to map brain circulation accurately, avoiding potential artifacts associated with manual perfusion.
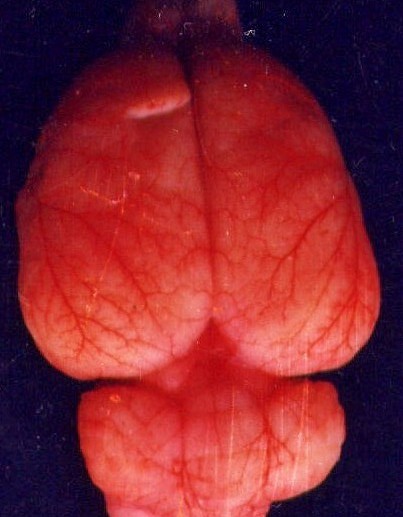
The rat's normal brain circulation
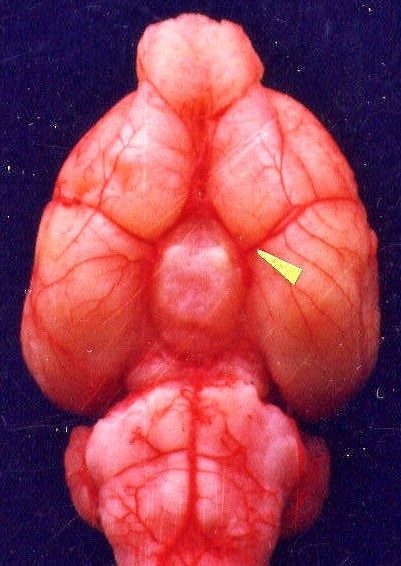
The bottom brain circulation
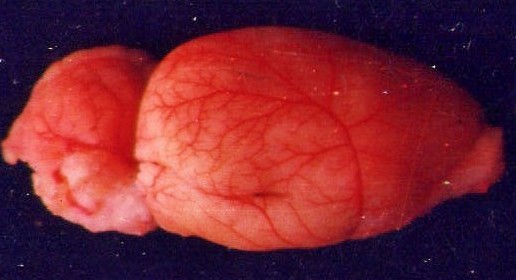
The side brain circulation
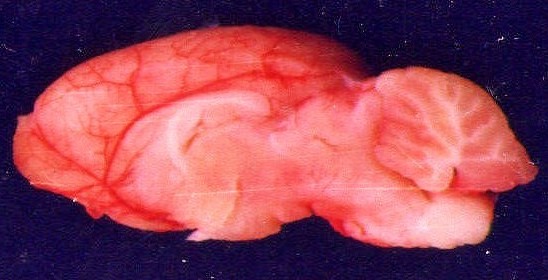
The inside brain circulation
In 367 rats, we performed surgical occlusion of the middle cerebral artery (MCAo), which created a distinct ischemic region. This clear-cut "window" allowed us to monitor whether any rescue blood flow could be introduced. After all, without blood, there is no life. The result of severing the artery was a stark, bloodless

The yellow arrow indicates the sever site of middle cerebral artery
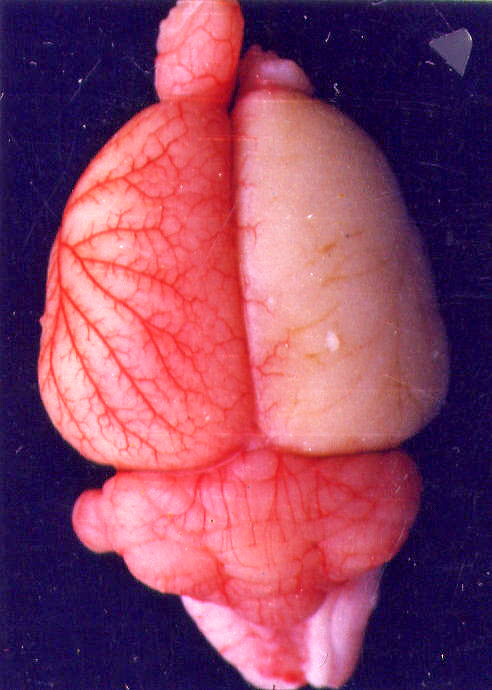
The result after Severing the artery.
If the acupuncture method was genuinely effective, we would expect to see new blood entering that white area.
Here are the results.
The findings from the acupuncture group astonished me. Below is a comparison of the effects in the acupuncture group versus the non-acupuncture group at 3, 6, 24, and 48 hours after MCAo.
3 Hours After MCAo
Non-acupuncture group on the left. Acupuncture group on the right.
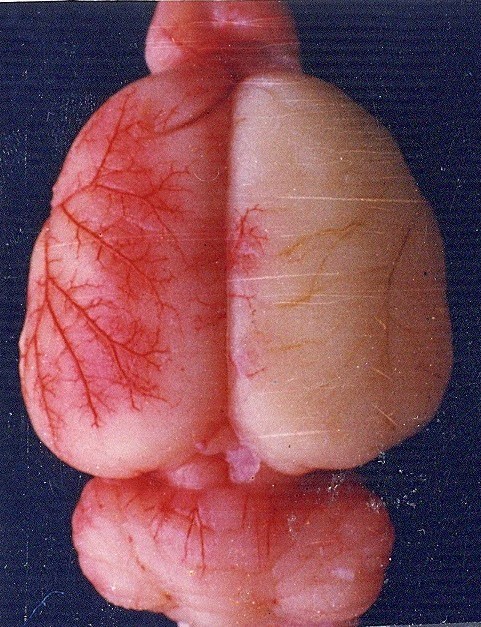
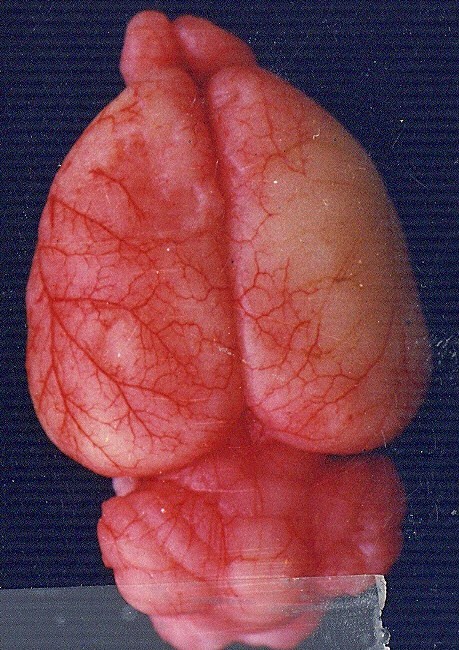
6 hours after MCAo
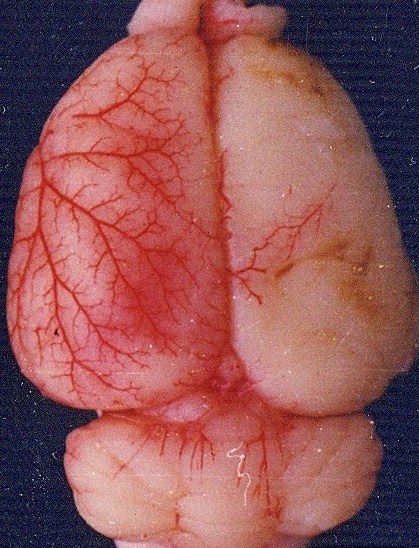
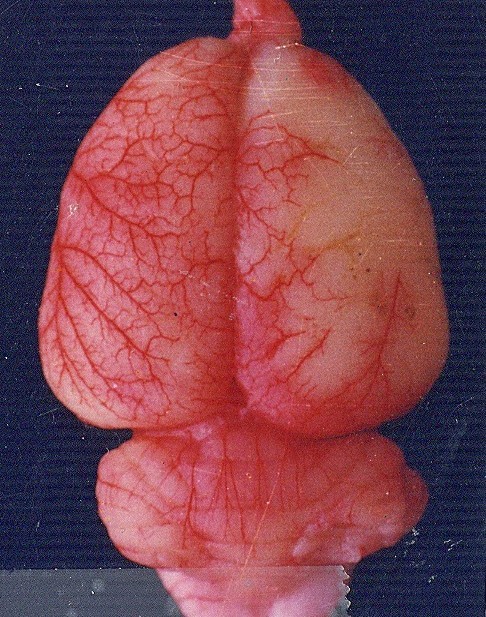
24 hours after MCAo
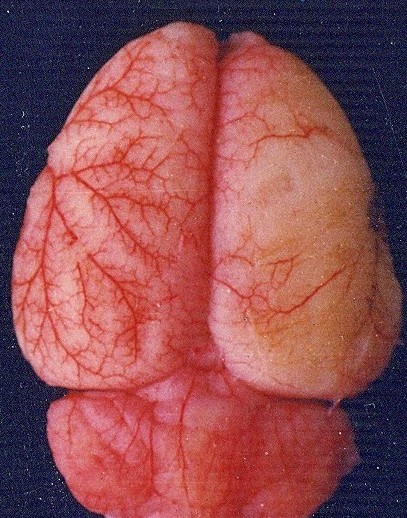
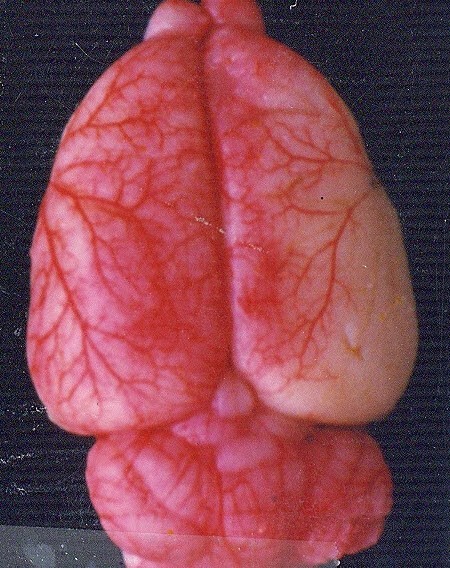
48 hours after MCAo
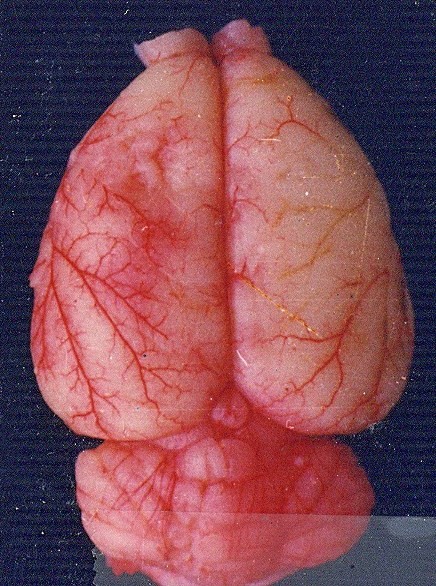
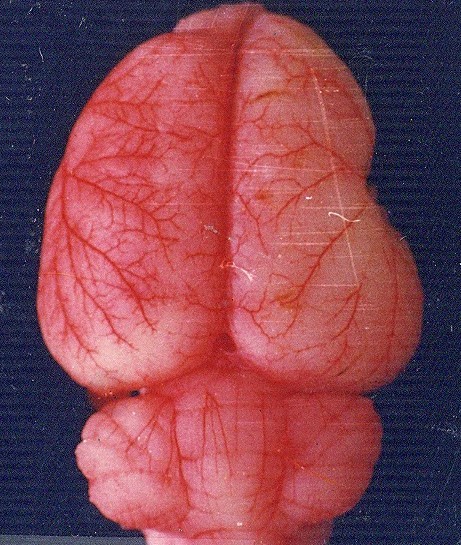
The results were clear: Yes, rescue blood entered the ischemic area. It arrived through a reverse flow, originating from the interconnected terminal branches of other major cerebral arteries—a network concentrated near the sagittal suture.
In a healthy brain, the middle cerebral artery (MCA) typically receives blood directly from the Circle of Willis. However, when the MCA was completely severed, our study revealed that an auxiliary network was immediately activated. This network provided a collateral pathway, supplying rescue blood to the compromised region.
This process is governed by the Circle of Willis, a critical circulatory structure at the base of the brain that connects all major cerebral arteries. It functions as a central hub to regulate blood supply. When a primary route like the MCA is blocked, the Circle of Willis can redirect blood pressure and flow. It pushes rescue blood through the connecting network at the ends of the arteries, enabling a reverse supply into the ischemic area.
This pivotal finding led to the next critical question: did this restored blood flow actually preserve the neurons?
To answer this, we pursued histochemical research to determine whether the neurons within the ischemic area were still alive.
The histochemistry results provided a definitive answer. Areas stained blue indicated live, functioning neurons. In stark contrast, the white areas represented zones of neuronal death caused by the complete occlusion of the middle cerebral artery (MCAo).
36 hours after MCAo without acupuncture
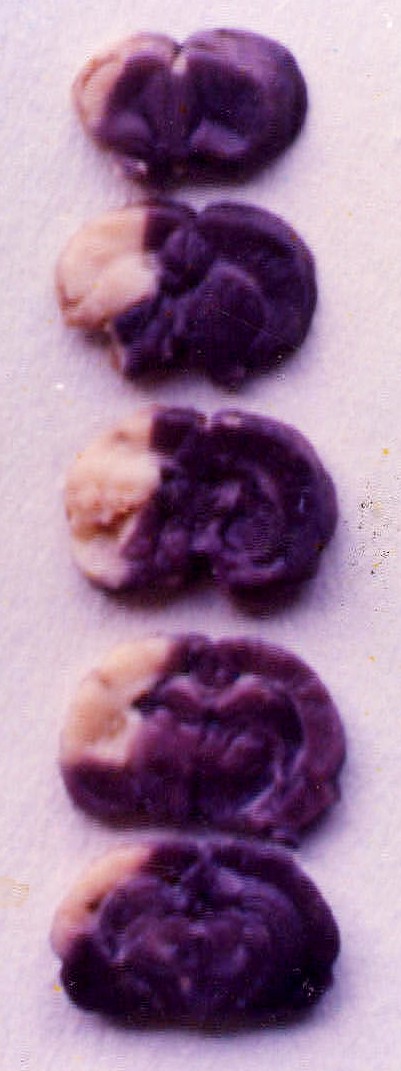
36 hours after MCAo with acupuncture

Five rats' brain showed the same result
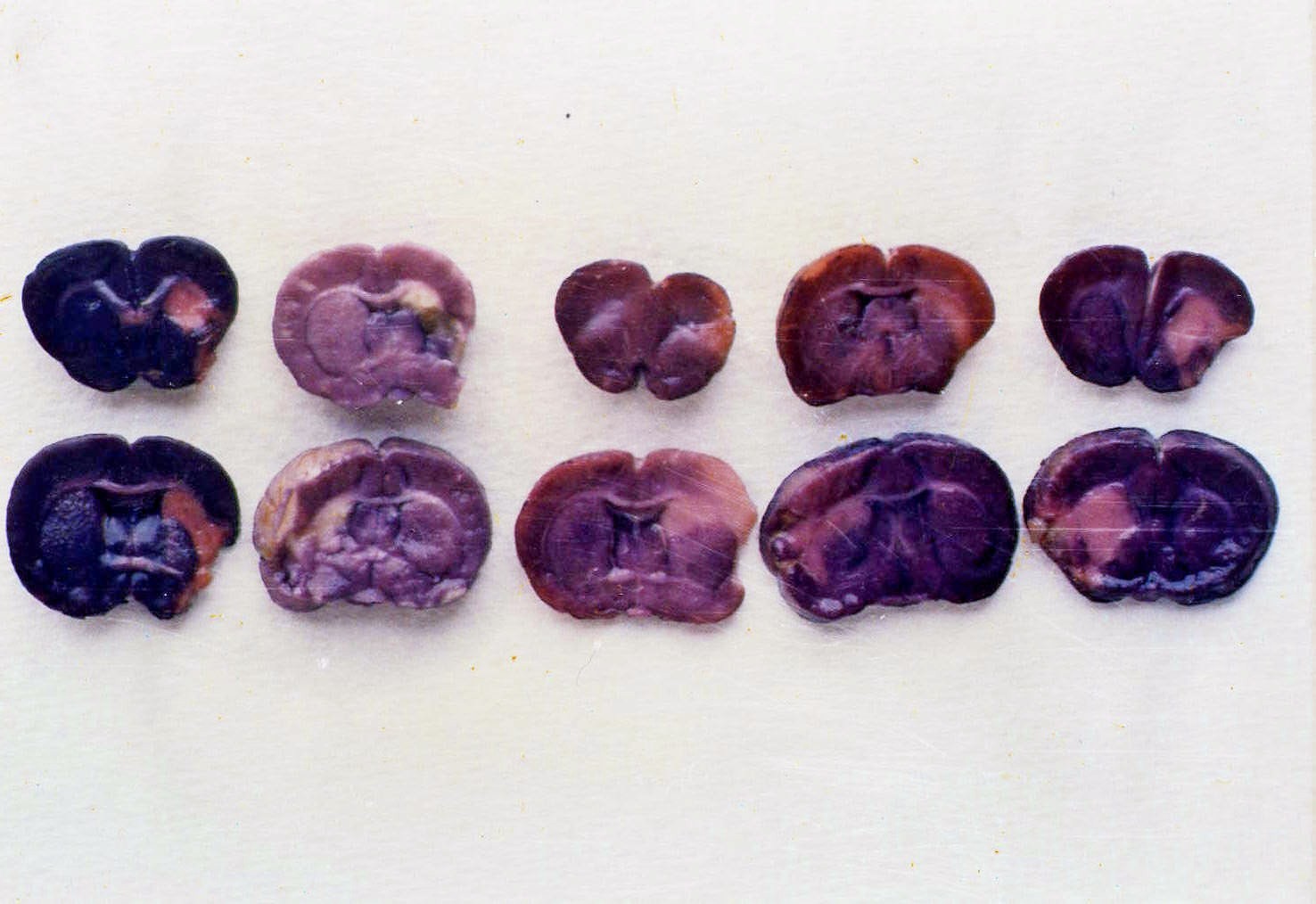
In the acupuncture group, a small white area persisted in the subcortex, indicating that the treatment's neuroprotective effect did not fully reach this region. This limitation is likely due to the inherently lower baseline blood circulation in the subcortical area compared to the cortex. The cerebral perfusion image below, taken under microscopy, illustrates this fundamental difference in vascular supply between the two regions.
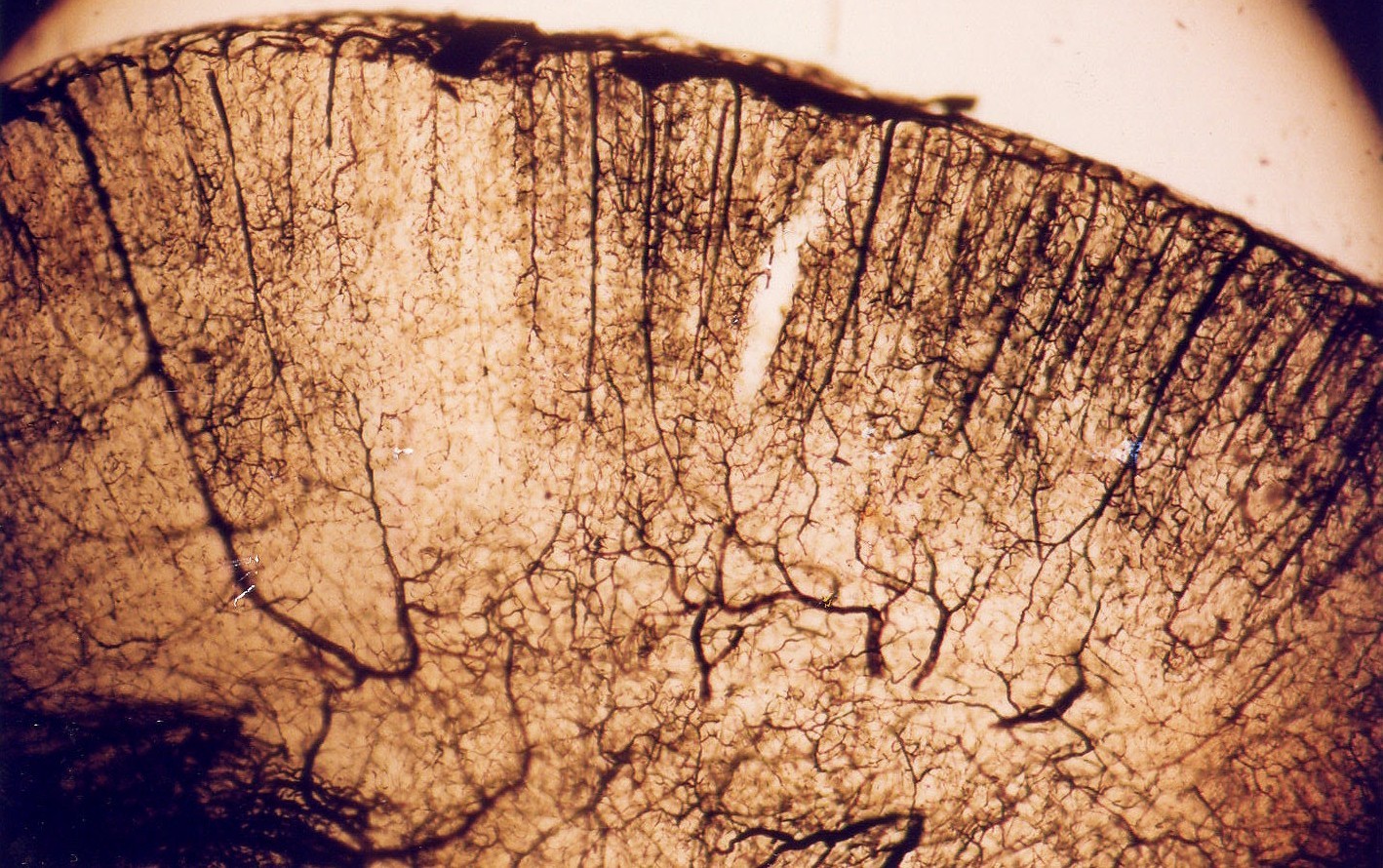
You might reasonably ask:
If this auxiliary network exists, why do people still suffer devastating strokes?
This is a vital point. In reality, a stroke is often the culmination of a slow, progressive process—years of systemic strain on the cardiovascular and neural systems. By the time the emergency occurs, the body’s inherent self-healing capacity is often depleted and insufficient to mount an adequate response.
This is precisely where our findings suggest acupuncture plays a critical role. It appears to act as a powerful systemic regulator and resource mobilizer. Rather than targeting just one area, acupuncture seems to coordinate a whole-body response. It prompts the cardiovascular system to work more efficiently, potentially increasing cardiac output and redirecting circulation to prioritize the brain.
In essence, acupuncture does not simply "add" something new; it empowers and optimizes the body’s existing self-healing systems during a crisis. By enhancing systemic coordination and circulation, it can help secure a far better recovery than the compromised body could achieve on its own.
Conclusion
My journey from skeptic to researcher revealed that acupuncture is not only effective for chronic conditions but also demonstrates remarkable potential as an adjunct therapy in acute emergencies, such as stroke.
Acupuncture by Dr. Na Zhai Springfield IL
1200 S 5th Street, Springfield IL 62703